Contact Us
What are Mouth ulcers and Canker Sores?
A mouth ulcer, also commonly referred to as Canker Sore, (although this is actually something different), is a small lesion in the mouth.
This can occur on the lips, tongue, gums, cheeks or on the roof of the mouth itself.
Mouth ulcers are incredibly common, with almost everyone having at least one in their life.
20% of people in the UK report regular mouth ulcers.
Regular mouth ulcers are likely due to an underlying condition called Aphtous Stomatitis.
The ulcer itself can be very painful on contact and can cause constant irritation.
If it is swollen it can interfere with one’s bite and be bitten on accidentally.
Mouth ulcers that occur on the cheek and gums are usually the most painful as these are the most likely to be bitten on.
Mouth ulcers can vary in size, being anything from 1mm to 1cm in diameter.
 Small ulcer on lip
Small ulcer on lip
Anything larger than 1cm in diameter may be cause for concern.
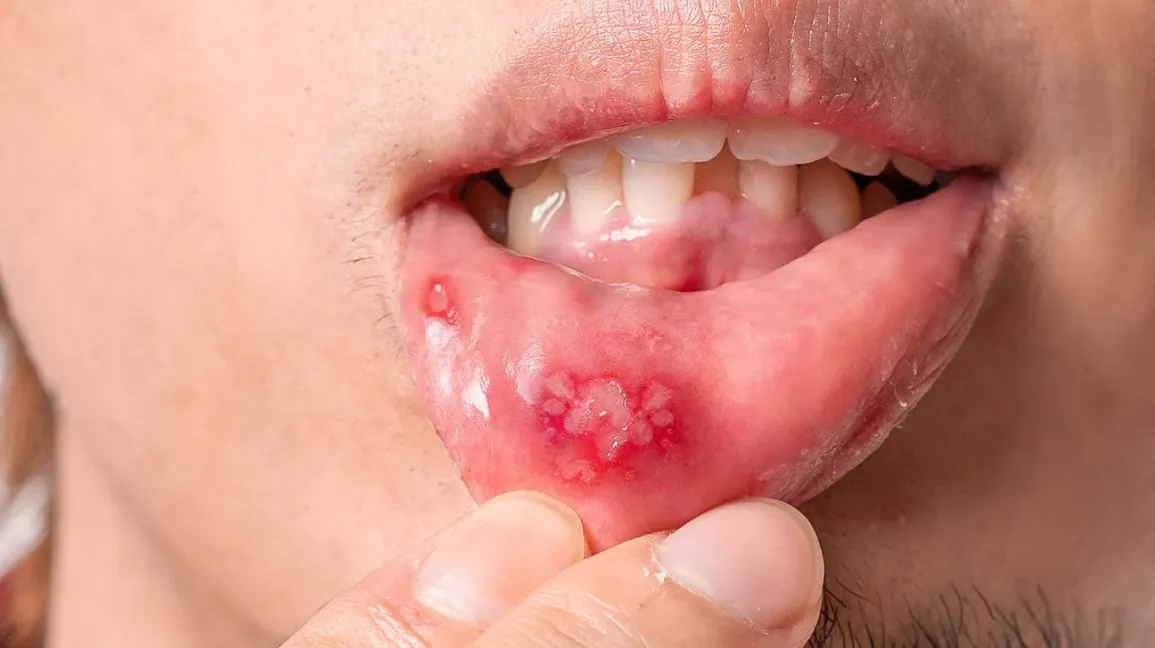
Mouth ulcers are usually a light yellowish colour in the centre. The outside of the ulcer can often be tinged bright red (brighter than the tissue that surrounds it).
This brightness is a result of inflammation, and the area can also be swollen.
Both Mouth ulcers and Canker Sores are non-contagious.
So what is the difference between a Mouth Ulcer and a Canker Sore?
The difference between a Mouth ulcer and a Canker Sore lies in its underlying cause.
Quite simply:
Mouth Ulcers are either caused by trauma to the mouth, or by a viral infection (most commonly Oral Herpes).
Canker Sores, on the other hand, are caused by an underlying condition called Aphthous Stomatitis.
If someone has Aphtous Stomatitis then they will likely have Canker Sores on a regular basis.
As many as 20% in the UK of people are thought to experience this.
Mouth ulcers and Canker Sores are virtually indistinguishable and can be managed and treated in the same way.
What causes Mouth Ulcers and Canker Sores?
Mouth ulcers
In the majority of cases mouth ulcers are caused by trauma to part of the mouth.
They are not normally indicative of any underlying medical condition.
This trauma can include:
- Cuts and scrapes inside the mouth from teeth or oral appliances (including braces, dentures and sleeping appliances)
- Burns from excessively hot or acidic foods
- Burns from stomach acid if you have acid reflux
- Injuries related to tooth grinding.
- Lacerations from habitual chewing of pens or other objects
 Cuts to the inside of the mouth caused by dental braces can cause mouth ulcers
Cuts to the inside of the mouth caused by dental braces can cause mouth ulcers
The ulcer forms as bacteria, often from tooth plaque, gets into the damaged area of the mouth and causes it to become infected.
As mouth ulcers are the result of infections in the mouth, they are more likely to occur if someone’s immune system is compromised.
Factors that compromise one’s immune system and have been linked to increased risk of mouth ulcers include:
- Poor diet – in particular deficiencies in Iron, Vitamin B12 or Vitamin C
- Lack of sleep
- Stress
- Autoimmune diseases (including HIV)
- Viral infections (including Oral Herpes- although this is more commonly associated with cold sores)
- Excessive alcohol consumption – Spirits can also damage tissue in the mouth on contact
- Undiagnosed food intolerances
- Smoking – hot smoke can also damage tissue in the mouth on contact
As ulcers often occur as the result of infection from plaque bacteria on the teeth, poor oral hygiene also plays a contributory role in the development of mouth ulcers.
Canker Sores
Canker Sores are specifically caused by an auto-immune condition called Aphthous Stomatitis.
Current thinking suggests that Aphthous Stomatitis makes a sufferer more prone to Canker Sores as it suppresses the immune system.
As the inside of the mouth regularly comes into contact with foreign organisms (food, bacteria in air etc), it is vulnerable to infection.
If someone’s immune system is suppressed then infection is more likely.
Thus inflammation and ulceration in the mouth can occur regularly
Unfortunately Aphthous Stomatis cannot be cured.
The condition is associated with no symptoms other than the regular development of Canker Sores.
The condition represents no serious harm to your long-term health.
As Canker Sores come as a result of an infection to damaged tissue in your mouth, you can reduce the risk of getting them by reducing the likelihood of damaging tissue in your mouth or by taking measures to reduce infection.
You can reduce the risk of damaging the soft tissue in your mouth by:
- Avoiding food that is overly hard, crispy or crunchy.
- Reducing your intake of overly sweet, sour or spicy food or drinks
- Drinking less fizzy drinks as these contain carbonic acid
- Not eating food that it is very hot (temperature-wise)
- Drinking as little alcohol as possible
- Wearing a night guard if you grind your teeth
- Brush with a soft bristled toothbrush
The risk of damage to the soft tissue in your mouth becoming infected can be minimised by:
- Maintaining as high levels of oral hygiene as possible: brush your teeth (twice) and floss daily, and regularly visit your dentist and hygienist
- Have a healthy diet to boost your immune system: in particular make sure you take on enough Vitamin C and Vitamin B12
- Avoid smoking as cigarette smoke itself can infect damaged tissue
- Rinse any sore part of your mouth with Corsodyl or a salt water solution
- Keep well hydrated to allow the body to flush out toxins efficiently
Following all these steps should reduce the amount of Canker Sores you get even if having Aphthous Stomatitis makes you predisposed to them.
How to treat Mouth ulcers and Canker Sores?
So long as they aren’t constantly being rubbed against or repeatedly bitten down on, ulcers should go away by themselves.
However the pain and interference with eating and talking that mouth ulcers and Canker Sores cause can mean that you want them gone as soon as possible.
Here is how its done:
1) Ulcers will disappear faster if they are not irritated or interfered with.
It therefore may be a good idea to avoid chewing on the side of the mouth where you have an ulcer (if possible).
Similarly you should try and to resist the urge to play with your ulcer with your fingers or tongue.
2) You can use over the counter painkillers to reduce the pain of your ulcer or canker sore.
The reduced pain should also decrease your urge to play with your ulcer. This should promote healing further.
Ideally you want to be using painkillers with an anti-inflammatory quality.
Anti-inflammatories fight infection as well as reduce pain, therefore making your ulcer or Canker Sore heal faster.
Ibuprofen (Advil or Neurofen) and Aspirin are the two most common over the counter anti-inflammatory painkiller.
Paracetamol is not an anti-inflammatory.
 Anti-inflammatories are best for reducing most painful oral health issues
Anti-inflammatories are best for reducing most painful oral health issues
3) Inflammation can be reduced by rinsing the ulcer with warm salty water.
This is because salt-water is a mild anti-septic. It can kill the harmful inflammation causing bacteria without doing any damage to the infected tissue itself.
Rinsing the ulcer out this way two or three times a day will promote healing and stop it from getting any worse.
 A Saltwater solution will gently disinfect your mouth ulcer
A Saltwater solution will gently disinfect your mouth ulcer
The salt water solution may taste unpleasant but it should not sting when coming into contact with your ulcer.
Some people assume that it will have the effect of “rubbing salt into an open wound” but this is simply not the case.
Many other home remedies have been bandied around the internet and forums, however only these three treatments have been scientifically proven to have work.
Purported remedies such as liquorice, lemon juice and black tea have no scientific backing.
Using proper treatments should help an ulcer or Canker Sore heal up to twice as quickly.
Is it worth going to a dentist because of an ulcer in my mouth?
As a general rule no.
 In the majority of cases, a dentist will be of little use in curing a mouth ulcer or Canker Sore
In the majority of cases, a dentist will be of little use in curing a mouth ulcer or Canker Sore
However there are definitely cases where a mouth ulcer or Canker Sore warrants a visit to the dentist.
1) If an ulcer is larger than 2cm in diameter (from one end to the other) than it may require surgical removal by an oral surgeon or dermatologist.
These Giant Ulcers will likely be incredibly painful, and may leave a scar post removal.
Regularly getting these ulcers may be the sign of a more serious underlying condition.
 Giant ulcer on back of the mouth
Giant ulcer on back of the mouth
2) If someone has more than 3 ulcers at any one time, than it is worth visiting a GP or dentist as this may be indicative of an underlying condition.
Such conditions may range from undiagnosed food allergies to auto-immune diseases such as HIV.
It is therefore important to seek medical advice if this happens to you.
3) If an ulcer or canker sore is causing an unbearable amount of pain, then it is a dental emergency.
Are mouth ulcers and Canker Sores a symptom of Oral Cancer?
99.9% of mouth ulcers are benign, and are not a symptom of cancer.
However, if you do have oral cancer, mouth ulcers that do not go away are a symptom.
Cancerous mouth ulcers usually appear under the tongue.
They can also appear in other parts of the mouth but this is less common.
 Even if you do have a resilient ulcer under your tongue, it is very unlikely to be related to cancer.
Even if you do have a resilient ulcer under your tongue, it is very unlikely to be related to cancer.
You should however have some cause for concern if you have such an ulcer in conjunction with risk factors for mouth cancer.
These are:
- Smoking
- Excessive alcohol consumption (regularly exceeding more than 21 units a week)
- Family history of oral cancer
- Having had the Human Papillomavirus (HPV) in the past
- Having a history of poor oral hygiene, particularly gum disease
If you think you may have oral cancer, please book a check-up with your dentist immediately.
What to do when children have mouth ulcers?
Mouth ulcers are very common in children.
They are particularly common in babies and toddlers from 0-3.
This is because the inside of their mouths are particularly soft, and they explore the world through putting new things in their mouths.
This can lead to damage to tissue in the mouth which can become infected and form ulcers.
Mouth ulcers can cause young children to become very irritable.
It can also make them not want to eat, drink water or have their teeth brushed due to the pain it causes.
 Mouth ulcers can cause a lot of pain and irritability in young children
Mouth ulcers can cause a lot of pain and irritability in young children
It can be hard to treat mouth ulcers in small children as treatment requires discipline.
In order to minimise the risk of your young child having mouth ulcers you should:
- Monitor and control what they put in their mouths
- Cut their nails regularly if they suck their thumb
- Make sure they have a healthy diet, particularly one that is high in Vitamin C and Vitamin B12
- Take them to the dentist if they have constant ulceration in their mouths.
Below is a useful video about how to manage mouth ulcers in children: